Dry Eye
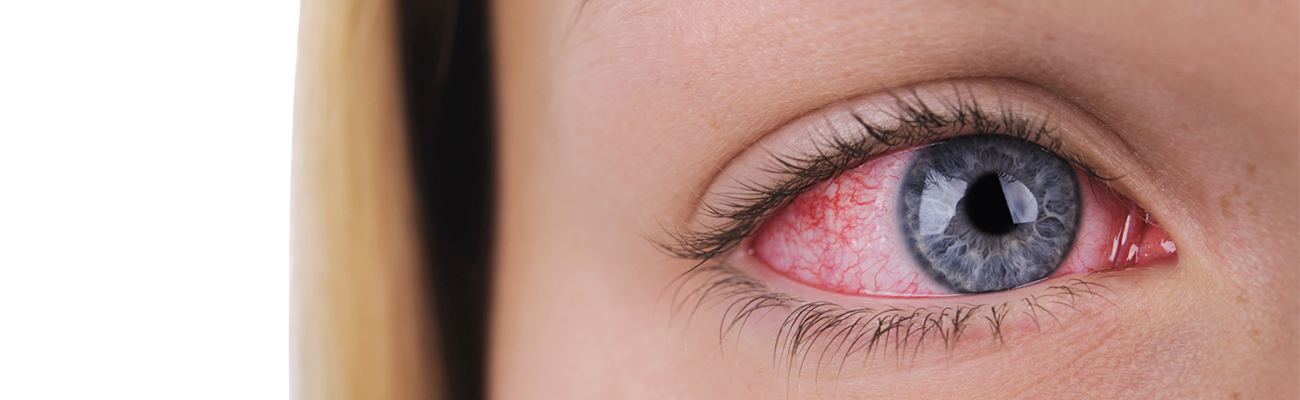

One of the more common causes of eye irritation is dry eye disease. The tear film lubricates the eye, smoothes irregularities for better vision, washes germs and other irritants from the eye surface and carries oxygen to the surface of the eye. “Dry eye disease” is a label for various disorders of the tear film, which is usually classified into two categories: decreased tear production, and excessive tear evaporation. In fact, most patients (50-70%) have both types of abnormality.
WHO IS AT GREATEST RISK?
Dry eye disease is more common with age and as body hormone changes occur, especially in post-menopausal women. Medications taken by mouth can cause dry eyes, including antihistamines, blood pressure medications, decongestants and antidepressants. Complaints of dry eyes are particularly common in patients with certain medical conditions such as Rosacea, arthritis and following eye surgeries. Certain autoimmune conditions, such as rheumatoid arthritis and lupus, occur together with dry eyes. The most severe form of dry eye is related to a condition known as Sjogren’s Syndrome. This condition affects several million people throughout the world. Not only are the eyes dry, but there is usually dryness of the mouth, nose or throat.
HOW IS DRY EYE DIAGNOSED?
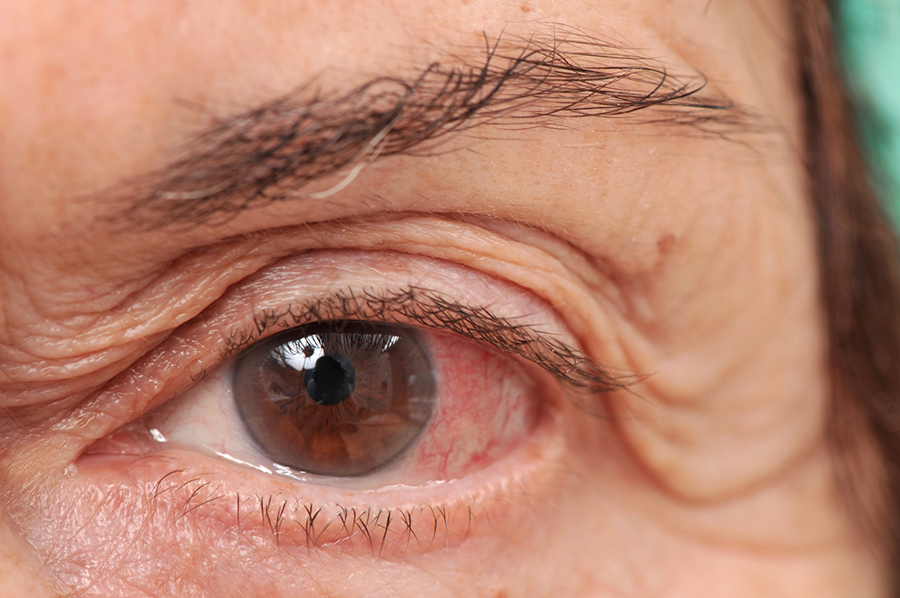


Many factors contribute to dry eyes. Most important is listening to a patient’s history. Patients typically complain of a collection of symptoms, which worsen as the day goes on:
- Sandy, gritty sensation
- Blurred vision
- Eye redness
- Foreign-body sensation
- Burning or stinging
- Contact lens intolerance
- Dryness
It is critical to identify eyelid abnormalities which may be present and contribute to symptoms of dry eye. Failing to correct eyelid problems often results in failure to relieve symptoms. A careful eye examination tests the quality, quantity and stability of the tears and to look for irritation of the eye surface.
These symptoms may be a result of tear underproduction, but more often, the cause is an abnormality of the eyelid oil-producing glands, a condition known as meibomian gland dysfunction (or meibomitis or blepharitis). The oils function to stabilize the tear film and slow evaporation (loss) of the protective tear film. Tear production and quality can be measured and oil quality can be assessed by examination. Other conditions occasionally are confused with dry eye, including allergies and diseases of the corneal surface. A careful eye examination tests the quality, quantity and stability of the tears and looks for these other conditions.
WHY IS PROPER DIAGNOSIS IMPORTANT?
If irritative symptoms are the result of both dry eye (tear under-production) and meibomitis (evaporative tear loss), and both conditions are not effectively treated, it is unlikely that symptoms will be relieved. It is critical for your eye care provider to identify eyelid abnormalities that may be present and contribute to symptoms of dry eye. Failing to treat this problem often results in failure to stabilize the tear film and failure to relieve symptoms. Even a perfect treatment plan for tear underproduction will not be sufficient to control meibomitis, and likewise, treatment for meibomitis will not completely relieve symptoms of tear underproduction. Effective treatment of both aspects of dry eye is necessary. I tell my patients that if their car has flat tires and an empty gas tank, just filling up the tank will not make the car ready to drive. All abnormalities must be effectively treated.
HOW IS DRY EYE TREATED?


We manage tear underproduction with a three-pronged strategy:
- Tear Supplementation
- Tear Stimulation
- Tear Retention
The mainstay of treatment for dry eyes is artificial tears, and these should always be tried first. The ideal tear lasts a long time and is comfortable without blurring. There is no one tear product that is ideal for everyone, but there are preferred choices for each type of dry eye, individualized for specific patient’s needs. Nighttime lubricating ointments are very useful. In severe cases, a lubricant can be prepared from a patient’s own serum, providing natural growth factors to the surface of the eye.
In addition to using artificial tears, it is helpful to make the most of the tears that are being produced. Wrap-around or glasses with side shields (moisture chambers) help retain moisture. There are some simple office procedures which can be extremely helpful for dry eyes, especially “punctal occlusion”. This is simply a way of sealing up the tear drainage so that tears are retained on the eye. This is similar to placing a plug in the drain in order to help a slow-running faucet fill the kitchen sink.
We manage meibomitis with a three-pronged strategy:
- Effective Eyelid Hygiene
- Pharmaceutical treatment of the eyelid oils
- Mechanical drainage of glands
- Thermal Pulsation (LipiFlow)
- Reopening (probing) of the meibomian gland ducts (where the oils exit)
Without good lid hygiene, it is unlikely that symptoms will be completely relieved. Instruction in effective methods to mobilize abnormally thick, stagnant and inflammatory oils is best done in person, as many patients perform this incorrectly or inadequately. We spend considerable time on this, one-on-one and using videos.
WHY TAUBER EYE CENTER?
EXPERIENCE AND EXPERTISE
More and more eye care providers are recognizing the impact of dry eye disease on the outcomes of other eye surgeries, such as cataract and laser correction (LASIK or PRK). If you have dry eye or have irritating eye symptoms, find out why and learn what you can do about it. If you have been advised to have cataract surgery or are choosing to have laser vision correction surgery, be sure that you do not have early dry eye or meibomian gland disease that may interfere with a good result.
Dr. Tauber is an internationally recognized authority on dry eyes and meibomitis and has been conducting research and lecturing in this field for over a decade. There is no substitute for an in-person consultation to discover the specific causes of dry eye for individual patients. Tauber Eye Center offers the most advanced testing and treatment of dry eye and meibomian gland dysfunction that is available anywhere. A visit with a true specialist is invaluable and will provide you with a great deal of information.